What is Post Laminectomy Syndrome?
Post Laminectomy Syndrome, is a generalized term used to describe the condition of patients who have not had a successful back or spine surgery results. Or patients who have experienced continued pain after surgery. Post laminectomy syndrome is also known as failed back syndrome (FBS). There is no equivalent term for FBS syndrome in any other type of surgery (e.g. there is no failed cardiac surgery syndrome, failed knee surgery syndrome, etc.).
There are many reasons a back surgery may or may not work. Even with the best surgeon and for the best indications, spine surgery is no more than 95% predictive of a successful result.
Reasons for Failed Back Surgery and Pain after Surgery
Spine surgery is basically able to accomplish only two things:
- Decompress a nerve root that is pinched, or
- Stabilize a painful joint.
Unfortunately, back surgery or spine surgery cannot literally cut out a patient’s pain. It is only able to change anatomy, and an anatomical lesion (injury) that is a probable cause of back pain. This pain must be identified prior to rather than after back surgery or spine surgery.
By far the number one reason back surgeries are not effective and some patients experience continued pain after surgery. One such reason is because the lesion that was operated on was not the cause of the patient’s pain.
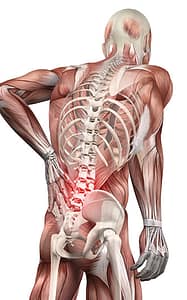
Post–Laminectomy Syndrome is characterized by residual and persistent back and/or leg pain following spine surgery.
Predictability of Pain after Surgery
Some types of back surgery are far more predictable in terms of alleviating a patient’s symptoms than others. For instance,
- A discectomy (or microdiscectomy) for a lumbar disc herniation that is causing leg pain is a very predictable operation. However, a discectomy for a lumbar disc herniation that is causing lower back pain is less likely to be successful.
- A spine fusion for spinal instability is a relatively predictable operation. However, a fusion surgery for multi-level lumbar degenerative disc disease is less likely to successfully reduce patient’s pain after surgery.
Therefore, the best way to avoid a spine surgery leading to an unsuccessful result is to stick to procedures with high degrees of success. As well as to make sure that an anatomic lesion that is amenable to surgical correction is identified preoperatively.
Other Causes of Post Laminectomy Syndrome
In addition to the above-mentioned causes of PLS, there are several other potential causes of a failed surgery, or continued pain after surgery:
- Fusion surgery considerations
- such as failure to fuse and/or implant failure,
- or a transfer lesion to another level after a spine fusion, when the next level degenerates and becomes a pain generator
- Lumbar decompression back surgery considerations
- such as recurrent spinal stenosis or disc herniation,
- inadequate decompression of a nerve root,
- preoperative nerve damage that does not heal after a decompressive surgery,
- or nerve damage that occurs during the surgery
- Scar tissue considerations (such as epidural fibrosis, which refers to a formation of scar tissue around the nerve root)
- Postoperative rehabilitation (continued pain from a secondary pain generator).
In addition to the primary reasons for post laminectomy syndrome, there are several reasons why a spinal fusion might fail. As in failing to alleviate a patient’s back pain after surgery, including fusion and implant failures, and transfer lesions.
Failure of Solid Fusion After Spine Surgery
When the fusion is for back pain and/or spinal instability, there is a correlation (although weak) between obtaining a solid fusion and having a better result of the spine surgery. If a solid fusion is not obtained through the spine surgery, but the hardware is intact and there is still good stability to the spine, the patient may still achieve effective back pain relief with the spine surgery. In many cases, achieving spinal stability alone is more important than obtaining a solid fusion from the spine surgery.
On postoperative imaging studies it is often very difficult to tell if a patient’s spine has fused. It can be even harder to determine if a further fusion surgery is necessary. In general, it takes at least three months to get a solid fusion, and it can take up to a year after the spine surgery. For this reason, most surgeons will not consider further spine surgery if the healing time has been less than one year. Only in cases where there has been breakage of the hardware and there is obvious failure of the spinal construct would back surgery be considered sooner.
Implant Failure in Spine Surgery
An instrumented fusion can fail if there is not enough support to hold the spine while it is fusing. Therefore, spinal hardware (e.g. pedicle screws) may be used as an internal splint to hold the spine while it fuses after spine surgery. However, like any other metal it can fatigue and break (sort of like when one bends a paper clip repeatedly). In very unstable spines, it is therefore a race between the spine fusing (and the patient’s bone then providing support for the spine), and the metal failing.
Metal failure (or hardware failure, implant failure), especially early in the postoperative course after back surgery, is an indicator of continued gross spinal instability. The larger a patient is and the more segments that are fused, the higher the likelihood of implant failure. Implant failure following spine surgery should be very uncommon in normal sized individuals with a one level fusion.
Transfer Lesion to Another Level after a Spine Fusion
A patient may experience recurrent pain many years after a spine fusion surgery. This can happen because the level above or below a segment successfully fused can break down and become a pain generator.
- This degeneration is most likely to happen after a two-level fusion (e.g. a fusion for L4-L5 and L5-S1 levels) and in a young patient (in the 30-50 year old age range).
- It is much less likely to happen if only the L5-S1 level is fused, as this segment typically does not have much motion. Fusing this level does not change the mechanics in the spine all that much.
- Most of the motion in the spine is at the L4-L5 level, and to a lesser extent at L3-L4. When the L4-L5 level is included in the spine fusion it transfers a lot of stress to L3-L4. This does not present as much of a problem for elderly patients. Since they tend to not be as active nor do they have the fusion for as many years.
- Transfer lesions are far more common in degenerative osteoarthritis conditions ( e.g. degenerative spondylolisthesis) and far less common in disc degeneration problems (e.g.degenerative disc disease or isthmic spondylolisthesis).
 Skip to content
Skip to content
