Many health factors can effect whether or not fractures are a risk in spinal osteoarthritis. Spinal osteoarthritis, osteoarthritis in general is more prevalent in women, is more common in women over 50; but can occur in men. OA related fractures in the spine may be an under-diagnosed result of spinal osteoarthritis. Fractures that do occur as a result of spinal OA can cause pain, changes in posture, and even limit independent function. Talking with your doctor about symptoms you experience related to osteoarthritis could help diagnose whether or not fractures are a risk.
Spinal Osteoporosis and Fracture Risk Factors
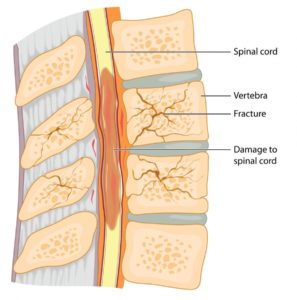 Due to hormonal changes, spinal osteoporosis is more common in patients over 50 years of age and four times more common in women than in men. It is worth noting that:
Due to hormonal changes, spinal osteoporosis is more common in patients over 50 years of age and four times more common in women than in men. It is worth noting that:
- It is believed that only 30% of vertebral compression fractures are actually diagnosed,4 indicating that spinal osteoporosis—and the resultant fractures—is more common than thought.
- Research shows 25% of all post-menopausal women in the United States have had a vertebral compression fracture from osteoporosis.5
- Vertebral compression fractures become more prevalent with age, with as much as 40% of women 80 years of age sustaining a vertebral compression fracture.5
- While less common in older men, who are not as prone to osteoporosis, compression fractures are also a significant problem.
Vertebral compression fractures not only cause physical symptoms, including pain and stooped posture, but can also be emotionally distressing to the patient, who may face some loss of independent function.
It is significant to note that both men and women suffer a significantly higher mortality rates after a compression fracture, although this is not necessarily a causal relationship; there are often numerous comorbid conditions and factors which could be responsible for the higher mortality rate.4
By: Grant Cooper, MD
04/03/2015
Continue reading the full article from Spine Health
