What Is Degenerative Disc Disease?
Degenerative disc disorder (DDD) is one of the most common causes of low back pain and neck pain. Degeneration of one or more intervertebral disc(s) is often called degenerative disc disease. It is a pathological process of uncertain causes that may cause acute or chronic back pain. Disc degeneration is a disease of aging, for most people is not a problem. In some people a degenerated disc can cause severe chronic pain if left untreated.
DDD symptoms can include pain and possibly radiating weakness or numbness stemming from a degenerated disc in the spine.
For most people the term degenerative implies the symptoms will get worse with age. However, the term does not apply to the symptoms, but rather describes the process of the disc degenerating over time.
Another source of confusion is created by the term disease, which is actually a misnomer. Degenerative disc disorder is not really a disease at all, but rather a degenerative condition that at times can produce pain from a damaged disc.
Disc degeneration is actually a natural part of aging. Over time all people will exhibit changes in their discs consistent with a greater or lesser degree of degeneration. However, not all people will develop symptoms. In fact, degenerative disc disease varies in its nature and severity.
What Causes It?
The pain associated with degenerative disc disorder is thought to stem from two main factors:
- Inflammation
The proteins contained within the disc space can cause inflammation, and as a general rule inflammation will cause pain. - Abnormal micromotion instability
If the outer rings of the intervertebral disc degenerates, it is not as effective in resisting motion in the spine. This is because it is usually not associated with gross instability, such as a slipped vertebral body or spondylolisthesis.
Both the inflammation and micromotion instability can cause lower back or neck muscle spasms. The muscle spasm is the body’s attempt to stabilize the spine. It is a reflex, and can be quite painful. Although the body’s response of muscle spasm is not necessary for the safety of the nerve roots.
The instability muscle spasms are thought to cause the flare-ups of intense pain often associated with degenerative disc disorder.
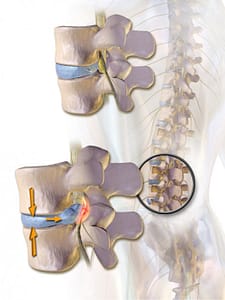
Degenerative disc disorder may cause acute or chronic low back pain.
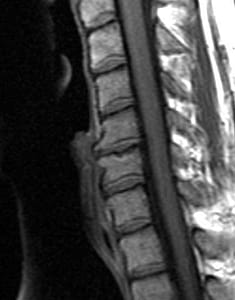
Typical radiographic findings in DDD are disc space narrowing, vacuum disc, end plate sclerosis, and osteophyte formation.
What Are Symptoms of DDD?
There are several symptoms that are fairly consistent for people with lower back pain or neck pain from degenerative disc disorder, including:
- Pain that is usually related to activity and will flare up at times but then return to a low-grade pain level, or the pain will go away entirely
- The amount of chronic pain, referred to as the patient’s baseline level of pain, is quite variable between individuals and can range from almost no pain/just a nagging level of irritation, to severe and disabling pain
- Severe episodes of back or neck pain that will generally last from a few days to a few months before returning to the individual’s baseline level of chronic pain
- Chronic pain that is completely disabling from degenerative disc disorder does happen in some cases, but is relatively rare
- Activities that involve bending, lifting, and twisting will usually make the patient’s pain worse
- Certain positions will usually make the pain worse. For example, for lumbar degenerative disc pain, the pain is generally made worse with sitting, since in the seated position the lumbosacral discs are loaded three times more than standing
- Walking, and even running, may actually feel better than prolonged sitting or standing
- Patients will generally feel better if they can change positions frequently
- Patients with lumbar DDD will generally feel better lying in a reclining position, or lying down with a pillow under the knees, since these positions relieve stress on the lumbar disc space
Severe Degenerative Disc Disorder Pain
Most patients with degenerative disc disorder will have some underlying chronic low back pain or neck pain, with intermittent episodes of more severe pain. The exact cause of these severe episodes of pain is not known, but it has been theorized it is due to abnormal micro-motion in the degenerated disc that spurs an inflammatory reaction. In an attempt to stabilize the spine and decrease the micro-motion, the body reacts to the disc pain with muscle spasms. The reactive spasms are what make patients feel like their back has “gone out.”
Specific Lumbar and Cervical DDD Symptoms
Degenerative disc disorder most commonly occurs in the cervical spine (neck) or the lumbar spine (lower back), as these areas of the spine have the most motion and therefore are most susceptible to wear and tear.
As a final note, it is helpful for patients to know that the amount of pain does not correlate to the amount of damage in the spine. Severely degenerated discs may not produce much pain at all, and discs with little degeneration can produce severe pain. What this means for patients is that even if they are experiencing severe pain, it does not necessarily mean that there is something seriously wrong with their spine and does not necessarily mean that they need surgery to repair any damage.
In general, the patient’s pain should not be continuous and severe. If it is, then other diagnoses must be considered.
 Skip to content
Skip to content
