Dr. Castillo’s thoughts about intrathecal pain pump management for treating back pain after surgeries. Intrathecal pain pump management is a proven safe and effective therapy for chronic pain control after back surgery.
I send a lot of patients for back surgery, when they have chronic back or neck pain. There are patients in danger of hurting a nerve in their spine which allows them to function. The purpose of back surgery is to fix a problem with the spine and stabilize the spine. Some people have no back pain after surgery, and we don’t talk about these outcomes. A lot of people are not so lucky. I tell all my patients, “Surgery is to fix pathology. Surgery is not to fix pain”. Most spine surgeons now warn patients before back surgery there is a great possibility of back pain after surgery. Many times, spine surgeons do not have a plan to deal with the pain following the surgery – which is where I come in.
Pain Control After Back Surgery
Intrathecal Pain Pump Management (IPPM) is an underutilized pain therapy in America. It is usually considered the last-ditch effort for controlling pain following: 1) just dealing with the pain, 2) taking oral opioids and other medications, and 3) trying Spinal Cord Stimulation therapy. Here is my take on each approach:
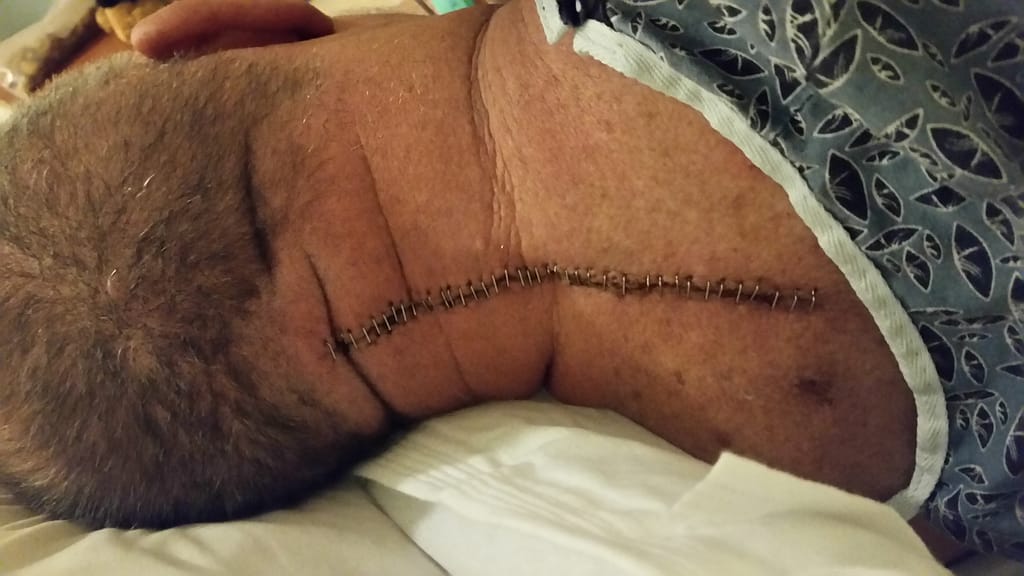
The patient pictured above had back surgery, and afterward was left with debilitating pain. Currently this patient has a pain pump which gives him pain control after back surgery; and allows him the ability to continue his daily activities and hobbies.
Deal With It
It is not as common now, but it is still a common “treatment method.” A surgeon states there is no problem with the surgery (and there probably wasn’t a surgical problem). “The pain will get better, but it will probably take three months.” Or “it will take six months.” “It might even take a year.” “There is nothing else I can do for your pain, you need to work with a pain physician.” In most Workman Compensation cases a patient is allowed to see a pain physician four times a year to get pain medications. But pain is not that simple, and each patient is different. Your pain is specific to you. If it affects your life it is a medical problem and, “deal with it,” is not a proper response.
Oral Opioids and other medications
A lot of patients are on at least one oral pain medication, an opioid like morphine. Pain can effect blood pressure and diabetes medications. Requiring most patients to take additional medications. These can be muscle relaxants, nerve meds (gabapentin or pregabalin), anxiety meds, and/or sleep meds. Some people may need a combination of all of these medications. New Federal and State limitations, do to the opioid crisis, have some patients suffering. The question is, do these medications have side effects? Yes. They all work on the brain to sedate parts of the brain; so patients can cope with their pain, but not relieve it. What doctors don’t know are the long-term effects of these medications on the brain and the body. When we wean patients off these medications; most state they didn’t know the extent of mental fog they were living in.
Spinal Cord Stimulation (SCS)
Every pain physician and stimulator company can show a study where SCS works for at least a year. A number of years ago, we did a study, for SCS pain control, for our office. We were going to taper 10 patients off their meds and trialed patients on SCS and IPPM. After tapering eight patients off medications and trying SCS and IPPM. All eight patients choose IPPM for pain control. Many SCS physicians stated SCS was never supposed to be a stand-alone therapy; it was meant to help oral opioids and other medications to control pain.
IPPM is not just another way to give opioids medications for pain control. Pain Pump Therapy manages pain directly at the spinal cord where the pain source can be found. A potential side effect, similar to oral opioids, is it may depress breathing at night. It is not a perfect pain control system, but a perfect system does not exist currently. With IPPM therapy the goal is to get the patient to a manageable pain level so they can live their life. A manageable pain level means some patients being able to go out to eat, travel, or do outdoor activities; as well as participate in daily activities like cooking or grocery shopping. A one week trial tells us if IPPM can be a treatment option. IPPM works in over 80% of our patients. I think it needs to be discussed before some spine surgeries.
by: Dr. Michael A. Castillo
 Skip to content
Skip to content
